The 1918 Influenza Pandemic, known colloquially as the Spanish Flu, represents one of the most devastating disease outbreaks in human history. Striki
The 1918 Influenza Pandemic, known colloquially as the Spanish Flu, represents one of the most devastating disease outbreaks in human history. Striking during the final year of World War I, this global catastrophe infected approximately one-third of the world’s population and resulted in an estimated 50 to 100 million deaths. The pandemic’s profound social, medical, and historical impact continues to influence how we understand and prepare for infectious diseases today.
This article delves into the origins, unique characteristics, societal effects, and lasting legacy of the 1918 Influenza Pandemic, offering insight into a crisis that reshaped the modern world.
The Origins: A Mystery Wrapped in a War
Identifying the true origin of the 1918 Influenza Pandemic/virus is challenging due to incomplete records and wartime censorship. While it became known as the “Spanish Flu,” Spain’s role was limited to open reporting rather than origination. Several theories exist:
- United States Hypothesis: Some researchers suggest that the virus first appeared in Haskell County, Kansas, in early 1918, spreading via military camps as the U.S. entered the war.
- France Hypothesis: Another theory posits that soldiers in France’s trenches contracted and spread the virus amid crowded, unsanitary wartime conditions.
- Asian Origins: Some studies suggest an origin in China or East Asia, but evidence remains inconclusive.
Despite these uncertainties, it is clear that the movement of troops during World War I accelerated the spread of the virus worldwide, turning a localized outbreak into a global catastrophe.
The Virus Itself: Deadly and Unusual
The causative agent of the pandemic was an H1N1 influenza A virus strain. However, unlike typical seasonal flu viruses, the 1918 strain had several unusual traits:
- High Mortality Among Young Adults: Influenza generally causes higher mortality in the very young and elderly, but the 1918 virus disproportionately killed healthy individuals aged 20-40, causing immense social and economic disruption.
- Rapid Disease Progression: Many patients deteriorated quickly, succumbing to viral pneumonia or secondary bacterial infections within days.
- Cytokine Storm: Modern research indicates the virus triggered a severe immune response known as a cytokine storm, where the immune system’s overreaction caused fatal lung damage.
The Three Waves: The Pandemic’s Deadly Rhythm
The pandemic occurred in three waves:
- First Wave (Spring 1918): This wave was relatively mild, with many people experiencing typical flu symptoms and recovering.
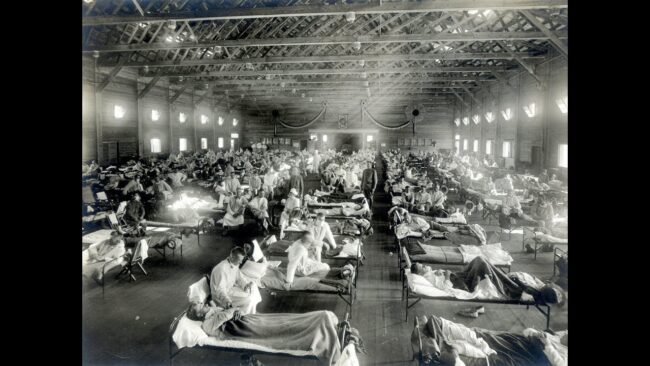
- Second Wave (Fall 1918): The most lethal phase, caused by a mutated, more virulent virus. Mortality rates soared, overwhelming healthcare systems globally.
- Third Wave (Winter 1918–Spring 1919): Though less intense than the second, this wave still caused significant illness and deaths before the pandemic subsided.
Worldwide Impact: A Crisis of Unprecedented Scale
The pandemic’s reach was global, affecting cities and rural areas alike:
- Infection Rates: Approximately 500 million people—about a third of the world’s population—contracted the virus.
- Death Toll: The pandemic claimed an estimated 50-100 million lives, more than the total fatalities of World War I.
- Vulnerable Populations: Indigenous peoples, remote communities, and populations with limited healthcare access experienced disproportionately high mortality rates.
- Economic Fallout: The pandemic disrupted labor forces, trade, and economies already weakened by war, leading to shortages and inflation.
- Urban Centers: Cities like Philadelphia and New York faced massive outbreaks, sometimes exacerbated by public events or delayed responses.
Social Disruption and Public Health Responses
The pandemic created fear and uncertainty worldwide:
- Public Health Measures: Governments implemented quarantines, closed schools and theaters, banned public gatherings, and mandated face masks.
- Variable Success: Cities that acted early and decisively, such as St. Louis, generally fared better than those that delayed interventions.
- Healthcare Challenges: Hospitals faced shortages of beds, staff, and supplies; many healthcare workers fell ill, further straining systems.
- Psychological Impact: The trauma of widespread death and isolation left lasting scars on communities and individuals.
Medical and Scientific Advances Inspired by the Pandemic
Though the 1918 virus predated the discovery of influenza viruses and antibiotics, the pandemic accelerated medical science:
- Epidemiology and Surveillance: The need for rapid disease tracking and reporting became evident, leading to better global surveillance systems.
- Vaccine Development: While no vaccine existed in 1918, research initiated in its aftermath laid the foundation for later influenza vaccines.
- Public Health Infrastructure: Countries recognized the importance of robust public health agencies and preparedness planning.
- Understanding Immune Responses: Studies of the cytokine storm phenomenon helped explain why healthy individuals were particularly vulnerable.
Lessons for Today and Tomorrow
The 1918 pandemic’s legacy offers critical lessons relevant to current and future health crises:
- Early Action Saves Lives: Timely implementation of control measures can reduce transmission and mortality.
- Transparency Builds Trust: Open communication from authorities is essential to manage public fear and misinformation.
- Global Cooperation Is Vital: Infectious diseases cross borders, requiring coordinated international responses.
- Investment in Healthcare Is Crucial: Strong health systems and research capabilities improve pandemic resilience.
- Preparedness Must Be Ongoing: Stockpiles, plans, and public education help mitigate future outbreaks.
These principles guided responses to later pandemics, including the 2009 H1N1 and COVID-19 crises, underscoring the 1918 pandemic’s enduring influence.
Conclusion
The 1918 Influenza Pandemic was a defining event of the 20th century that reshaped society and medicine. Its staggering death toll and unique epidemiological features challenged humanity and exposed vulnerabilities in health systems. However, it also catalyzed advances in science and public health infrastructure that continue to save lives.
Understanding the 1918 pandemic’s causes, consequences, and lessons is essential for preparing for future infectious disease threats. Remembering this global tragedy honors those lost and inspires a commitment to vigilance, cooperation, and innovation in protecting public health worldwide.
Frequently Asked Questions (FAQs)
Q1: Why is the 1918 flu called the “Spanish Flu” if it didn’t start in Spain?
A1: Spain’s neutral stance in World War I allowed uncensored reporting of the outbreak, making it appear as the epicenter despite likely originating elsewhere.
Q2: How many people died during the 1918 pandemic?
A2: Between 50 million and 100 million deaths globally, making it one of the deadliest pandemics in recorded history.
Q3: Why did the virus kill so many healthy young adults?
A3: The virus triggered a cytokine storm, an overactive immune response that caused severe lung damage, disproportionately affecting healthy individuals.
Q4: How did World War I influence the pandemic?
A4: Troop movements, crowded conditions, and wartime disruptions facilitated rapid, worldwide spread of the virus.
Q5: Were there any vaccines or treatments at the time?
A5: No vaccines or effective antiviral treatments existed; care was supportive only.
Q6: What public health actions helped reduce transmission?
A6: Early quarantines, social distancing, school closures, mask mandates, and public gathering bans helped curb spread when implemented promptly.
Q7: Did all countries experience the pandemic the same way?
A7: No. Mortality and infection rates varied widely based on factors like healthcare access, public health responses, population density, and socioeconomic status.
Q8: What are the main lessons from the 1918 pandemic?
A8: Early intervention, transparent communication, strong health infrastructure, investment in research, and international cooperation are vital for pandemic preparedness.
Must Visit: onlinemrkting



COMMENTS